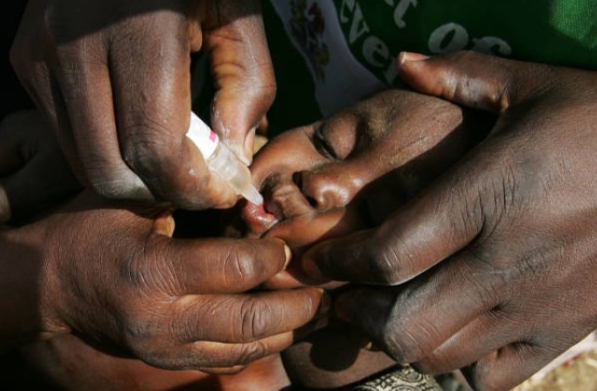
Malaria Vaccine in Africa: Hope for Eradicating Malaria in African Children
Malaria Vaccine in Africa: A Ray of Hope for Children’s Survival and Continental Health Transformation
In 2019, the World Health Organization (WHO) launched a pilot program to implement the malaria vaccine in Africa. For this purpose, Malawi, Kenya, and Ghana were selected to administer the first doses of the pilot program to children as young as 5 months old. The pilot introduction programs for the “RTS, S” vaccine have allowed over 1.7 million children to receive at least one dose of the vaccine. This initiative has sparked hope among many populations and nations affected by malaria, which remains the leading cause of mortality in Sub-Saharan Africa.
Malaria continues to be a significant scourge, especially for children, due to increasing resistance to treatments. It is important to note that malaria holds a unique place in history. In the 20th century alone, malaria was responsible for nearly 5% of human deaths, according to researchers. Two years ago, Gavi approved the implementation of a malaria vaccination program in African countries where malaria is endemic. This research, which has taken decades to develop a vaccine against this formidable health enemy in many of our environments, will bring relief to affected populations.
Malaria is caused by a parasite, Plasmodium, transmitted to humans through the bites of infected female Anopheles mosquitoes. The first symptoms typically appear within 15 days of the infectious bite. When treated promptly, most patients recover fully. However, malaria diagnosis is often delayed because initial symptoms such as headaches, fever, and chills can be mistaken for signs of other illnesses.
Without treatment, malaria caused by Plasmodium falciparum can worsen rapidly and lead to death within 24 hours. The number of malaria cases reached 241 million in 2020, resulting in 627,000 deaths (WHO REPORT DECEMBER 2021), with over two-thirds occurring in children under 5 years old, most of whom are in Sub-Saharan Africa. Plasmodium falciparum remains the predominant species, accounting for over 95% of malaria-related deaths, alongside four other species.
The hope of eradicating malaria on the continent is a dream that many have been waiting for, especially since Gavi, WHO, and UNICEF announced the allocation of 18 million doses of malaria vaccine to twelve African nations for the period 2023-2025. The first doses are expected to be administered in early 2024. This allocation is likely to constitute a crucial step in the fight against one of the main causes of death on the continent.
The twelve countries set to introduce the malaria vaccine this year include Benin, Liberia, Niger, Cameroon, Democratic Republic of Congo, Uganda, Burkina Faso, Burundi, and Sierra Leone. It is important to note that the allocation of these doses is determined in accordance with the principles outlined by the Allocation Framework (which is based on ethical principles and solidarity) for limited vaccine stocks, prioritizing areas with the greatest needs and where the risk of malaria-related disease and death in children is high, and access to treatment is challenging.
Cameroon, the first country outside the pilot countries, received its batch of 330,000 vaccine doses in late November (marking the transition from the pilot phase to routine use). The country is preparing to launch the vaccination phase in the first quarter of 2024 through other routine vaccination programs supported by Gavi. Other countries are still awaiting the deployment of doses to launch their campaigns in the first quarter.
We know that introducing a new vaccine into vaccination programs requires significant preparation, including training of healthcare workers, investments in infrastructure, technical and storage capacity enhancement, community mobilization, and awareness. The malaria vaccine comes with an additional challenge as it requires a four-dose protocol with a spaced-out schedule, necessitating careful planning, strong awareness efforts, logistical organization, and a competent healthcare team to ensure effective distribution.
What will be the impact of this long-awaited vaccine on the continent?
This vaccine could have a significant impact on the fight against malaria. The malaria vaccine represents a major advancement in the health and survival of children, families, and communities. The primary impact is the reduction of morbidity, especially among vulnerable groups. Additionally, it improves the quality of life by decreasing malaria-related morbidity. This initial dose primarily targets children at risk of malaria-related deaths, providing them with a better chance of survival. The goal is to meet the continental demand, and we hope that the supply can further increase to allow a large number of children to benefit from this scientific advancement that could save their lives, while we await its expansion to adults.
How much does this vaccine cost?
According to sources from the Ministry of Health in Cameroon, the RTS, S vaccine, commercially known as Mosquirix, was procured through Gavi. Regarding the financing of this vaccine, it should be noted that the dose is normally priced at $9.7 USD, but in consideration of the government’s request to the vaccination alliance, Cameroon will contribute $0.2 USD per dose. Other countries will also receive substantial doses for their national malaria control programs, negotiated with Gavi.
However, challenges persist, particularly in terms of accessibility and cost that different governments will need to include in their budgets, as well as logistical implementation for a large-scale vaccination effort. While the malaria vaccine offers great hope, it is important not to overlook national malaria control programs (NMCPs), which provide an integrated approach to other interventions such as insecticide-treated bed nets and malaria treatment protocols tailored to each country’s parasite strains for effective malaria control.
